Essential Takeaways
 Breast density is a normal part of your anatomy and plays an important role in how your screenings are interpreted.
Breast density is a normal part of your anatomy and plays an important role in how your screenings are interpreted.- Dense breast tissue is common and can affect how clearly abnormalities appear on imaging tests.
- Knowing your density helps guide more personalized breast cancer screening decisions.
- A 3D mammogram and other tools may be recommended to improve detection, depending on your density.
- Staying informed supports better preventive health screening and long-term peace of mind.
Taking Charge of Your Breast Health
If you have ever read your mammogram report and felt confused by the term “breast density,” you are not alone. Many women receive this information without much explanation, leaving them unsure about what it means for their health. It can feel unsettling to hear that you have dense breast tissue, especially if you are already thinking about your cancer risk.
The truth is, breast density is one natural aspect of your body. It does not mean something is wrong, but it does influence how your screenings are performed and interpreted. By taking the time to understand it, you empower yourself to make informed and confident choices about your care.
Let’s look at what breast density categories mean, how they relate to mammogram risk factors, and what steps you can take to feel more in control of your health.
What Are Breast Density Categories?
Your breast density categories describe the ratio of glandular and fibrous tissue compared to fatty breast tissue. These categories come from what shows up on a mammogram, and they fall into four groups: almost entirely fatty, scattered density, heterogeneously dense, and extremely dense.
This is an important part of understanding breast tissue because each type appears differently on imaging. Fatty tissue shows up darker, while dense tissue appears white. Since potential abnormalities also appear white, a higher density can make it more difficult to detect changes.
According to the Centers for Disease Control and Prevention, about half of women aged 40 and older have dense breasts. This makes dense breast awareness an essential part of patient education on breast health. Knowing your category helps you and your provider decide whether additional imaging may be helpful.
How Breast Density Affects Mammogram Results
Breast density plays a significant role in the effectiveness of your screening. A traditional mammogram is a powerful tool, but its accuracy can be limited in women with dense tissue.
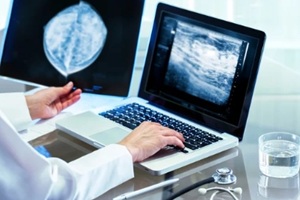 Research shows that mammography sensitivity can decrease in dense breasts, sometimes missing small abnormalities that could be easier to detect in less dense tissue. This is one reason why understanding your density is so important when evaluating mammogram risk factors.
Research shows that mammography sensitivity can decrease in dense breasts, sometimes missing small abnormalities that could be easier to detect in less dense tissue. This is one reason why understanding your density is so important when evaluating mammogram risk factors.
A 3d mammogram, also called a digital breast tomosynthesis, can improve detection by creating layered images of the breast. This allows radiologists to examine tissue more closely and reduces the risk that overlapping structures will obscure an abnormality. Many providers now recommend this option as part of a more advanced breast imaging guidance strategy.
Breast Density and Cancer Risk
It is natural to wonder how density affects your overall risk. Having dense breast tissue means your breast cancer risk is a bit higher than if your breasts were mostly fatty tissue.
A study in the American Journal of Epidemiology found that women with extremely dense breasts may have a risk that is about 1.8 times higher than women with average density. While this may sound concerning, it is important to remember that density is just one factor in a broader breast cancer risk assessment.
Things such as age, family history, lifestyle, and genetics can also play a role. By understanding how these pieces fit together, you and your provider can create a screening plan that reflects your individual needs.
Screening Options for Dense Breasts
If you have been told you have dense breasts, you may benefit from additional screening methods alongside your routine mammogram. These options are designed to improve detection and provide reassurance.
Ultrasound is commonly used as a tool in follow-up appointments to evaluate specific areas more closely. It can help distinguish between solid masses and fluid-filled cysts, offering valuable insight when mammogram results are unclear.
Magnetic resonance imaging, or MRI, may also be recommended in certain higher-risk cases. According to the American Cancer Society, MRI can detect cancers that mammography may miss, particularly in women with increased risk factors.
Schedule an Appointment With Raleigh Gynecology & Wellness
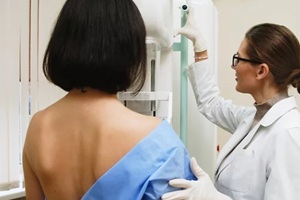 It is completely normal to feel overwhelmed when reviewing breast health information. You may be balancing a busy schedule, family responsibilities, and your own health at the same time. Taking time to understand your body is a powerful act of self-care.
It is completely normal to feel overwhelmed when reviewing breast health information. You may be balancing a busy schedule, family responsibilities, and your own health at the same time. Taking time to understand your body is a powerful act of self-care.
If you have questions about your breast density or need help choosing the right screening plan, our compassionate women’s health team is here for you. Schedule your appointment with Raleigh Gynecology & Wellness today and take control of your health with confidence.

 Genetic counseling helps individuals and families understand their odds of inheriting certain health conditions.
Genetic counseling helps individuals and families understand their odds of inheriting certain health conditions. Research estimates that about
Research estimates that about 
 There is no strong scientific evidence that
There is no strong scientific evidence that  Skin irritation or chafing
Skin irritation or chafing Misinformation can quickly spread, especially when it taps into fears about cancer or toxins. The truth is that there is no strong scientific evidence linking underwire bras to lymphatic blockage or breast cancer.
Misinformation can quickly spread, especially when it taps into fears about cancer or toxins. The truth is that there is no strong scientific evidence linking underwire bras to lymphatic blockage or breast cancer. A
A 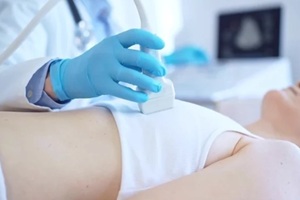 Many women have dense breasts, in which fibrous and glandular tissue make up a greater proportion of the breast than fatty tissue. Dense tissue can make it challenging for mammograms to differentiate between normal and abnormal areas because both dense breast tissue and potential tumors appear white on mammograms.
Many women have dense breasts, in which fibrous and glandular tissue make up a greater proportion of the breast than fatty tissue. Dense tissue can make it challenging for mammograms to differentiate between normal and abnormal areas because both dense breast tissue and potential tumors appear white on mammograms.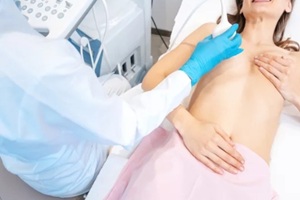 Knowing your breast imaging options can help you feel more in control of your health and choices. Ultrasound for breast health is a safe, practical tool that provides valuable information when used alongside diagnostic mammography. It can help clarify suspicious findings and guide further care in a way personalized to you.
Knowing your breast imaging options can help you feel more in control of your health and choices. Ultrasound for breast health is a safe, practical tool that provides valuable information when used alongside diagnostic mammography. It can help clarify suspicious findings and guide further care in a way personalized to you. Mammograms can be safely performed during or after breastfeeding when medically indicated, and there is no need to interrupt lactation.
Mammograms can be safely performed during or after breastfeeding when medically indicated, and there is no need to interrupt lactation. Breastfeeding causes increased breast density because your milk ducts and glands are fuller and more active.
Breastfeeding causes increased breast density because your milk ducts and glands are fuller and more active.  If you’re pregnant, breastfeeding, recently postpartum, or juggling it all and have questions about mammography, breast cancer screening, or breast health concerns, we’re here for you.
If you’re pregnant, breastfeeding, recently postpartum, or juggling it all and have questions about mammography, breast cancer screening, or breast health concerns, we’re here for you.