Essential Takeaways:
- Perimenopause can start earlier than most women expect, sometimes in the late 30s or early 40s.
- Early symptoms often feel “random,” making them easy to dismiss or misinterpret.
- Hormonal fluctuations can affect your cycle, sleep, mood, and body in subtle ways.
- Tracking symptoms can help you recognize patterns and advocate for your health.
- A supportive perimenopause doctor can guide you through diagnosis and treatment options.
Spotting the First Shifts
 Perimenopause is one of those transitions that most women hear about, but few feel fully prepared for. Surprise mood swings, irregular periods, and other early symptoms can appear without warning. Many women describe this stage as feeling “off,” “different,” or “not like myself,” but they aren’t always sure why.
Perimenopause is one of those transitions that most women hear about, but few feel fully prepared for. Surprise mood swings, irregular periods, and other early symptoms can appear without warning. Many women describe this stage as feeling “off,” “different,” or “not like myself,” but they aren’t always sure why.
This uncertainty can be frustrating, especially if symptoms are misunderstood or brushed off. Working with a knowledgeable perimenopause doctor can make the process feel more manageable and far less confusing.
Perimenopause in Plain Terms
Perimenopause is the transitional period that leads up to menopause, when the ovaries are no longer capable of ovulating. During this transition women experience changes in production of their reproductive hormones, primarily progesterone and estrogen. This shift doesn’t happen overnight. In fact, it can last an average of four to eight years.
During this time, hormone levels don’t simply drop but fluctuate. That means symptoms can appear and disappear or change in intensity, which is part of what makes perimenopause so confusing. One month, everything may feel “normal,” and the next, small changes suddenly stand out.
Irregular Periods Are Often One of the First Signs
Even women with historically predictable cycles can begin noticing changes. Periods may begin earlier or later than expected, become lighter or heavier, or skip entirely. These shifts can feel unsettling, especially if you’ve always had a consistent rhythm.
Irregular periods happen when the ovaries release eggs less consistently, creating unpredictable patterns of hormone production. While changes to your cycle alone don’t confirm perimenopause, they’re one of the most common early indicators.
Hot Flashes and Night Sweats
Hot flashes can start during perimenopause, not just menopause. At first, they may be mild, infrequent, or so subtle you’re not sure whether to label them “hot flashes” at all. Many women report feeling sudden warmth in the chest, face, or neck, followed by sweating or a brief chill after.
Night sweats can be especially disruptive since they interrupt sleep, leaving you groggy and irritable the next day. Even if they happen only occasionally, they are a strong sign that hormone levels are shifting.
Sleep Disturbances and Fatigue
If you’re waking up at 3 AM for no apparent reason, or struggling to fall asleep despite being tired, you’re not alone. Hormonal changes affect the body’s internal clock, making it harder to get refreshing, uninterrupted rest.
Some women lie awake with racing thoughts. Others drift off easily but wake multiple times through the night. Over time, poor sleep leads to daytime fatigue, reduced focus, and irritability. As sleep issues can stem from many causes, this symptom is another one that’s often overlooked or blamed on stress.
Mood Changes and Emotional Sensitivity
 Women often describe themselves as “more reactive,” “more sensitive,” or simply “not feeling like myself.” Minor frustrations may feel bigger. You might cry more easily or feel irritable or anxious without an apparent trigger.
Women often describe themselves as “more reactive,” “more sensitive,” or simply “not feeling like myself.” Minor frustrations may feel bigger. You might cry more easily or feel irritable or anxious without an apparent trigger.
These emotional shifts aren’t a sign of weakness but rather a biological response to fluctuating estrogen levels, which play a significant role in regulating neurotransmitters such as serotonin. Mood changes can be subtle at first, but when they start interfering with daily life, it’s a good time to reach out for guidance.
Changes in Libido and Sexual Comfort
As estrogen levels change, so does vaginal tissue. Some women notice decreased lubrication, light discomfort during intercourse, or increased sensitivity. Others experience a change in libido, sometimes lower and other times higher.
These symptoms are common and can often be managed with supportive care solutions, such as lubricants, hormonal options, or other treatments that restore comfort and confidence.
Physical Changes You Might Not Expect
Some early signs appear more quietly and are easy to attribute to aging, stress, or lifestyle changes:
- Tender or swollen breasts
- Weight changes, especially around the midsection
- Headaches or increased migraines
- Hair thinning or dryness
- Joint stiffness
- Heart palpitations
Individually, these symptoms may not seem hormonal. Together, however, they can paint a clearer picture.
When to Seek Support
You don’t have to wait for symptoms to become disruptive. If you’re noticing consistent physical or emotional changes, especially between your late 30s to early 50s, speaking with a women’s health provider can help you get ahead of the transition.
- A woman’s health team can help with:
- Symptom evaluation
- Personalized treatment options
- Lifestyle and nutritional guidance
- Supportive therapies for sleep, mood, and cycle changes
- Hormone testing when necessary
Most importantly, you’ll gain clarity and reassurance, which can make a tremendous difference in how you feel day to day.
Take the Next Step: Raleigh Gynecology & Wellness is Here to Help
 If you’re experiencing changes that don’t feel like “you,” our women’s health specialists are ready to support you through every stage of perimenopause.
If you’re experiencing changes that don’t feel like “you,” our women’s health specialists are ready to support you through every stage of perimenopause.
Schedule an appointment today at Raleigh Gynecology & Wellness to get clear answers, compassionate care, and a plan that helps you feel more in control of your health.

 You’re going about your day, juggling family, work, and just trying to find a moment to breathe, when you suddenly notice something new. Your heart feels as though it’s racing. Or maybe you have fatigue that won’t quit, sudden night sweats, or a strange flutter in your chest that has you wondering if it’s stress, hormones, or something more.
You’re going about your day, juggling family, work, and just trying to find a moment to breathe, when you suddenly notice something new. Your heart feels as though it’s racing. Or maybe you have fatigue that won’t quit, sudden night sweats, or a strange flutter in your chest that has you wondering if it’s stress, hormones, or something more.
 Menopause marks a transition that encourages women to focus more on self-care and preventive health. By staying informed and proactive, you can significantly reduce your risk of heart-related conditions and improve your quality of life.
Menopause marks a transition that encourages women to focus more on self-care and preventive health. By staying informed and proactive, you can significantly reduce your risk of heart-related conditions and improve your quality of life.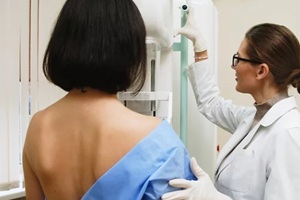 National programs such as the CDC’s NBCCEDP provide free or low-cost
National programs such as the CDC’s NBCCEDP provide free or low-cost  Regular breast cancer screenings are one of the most effective ways to detect disease early, often before symptoms appear.
Regular breast cancer screenings are one of the most effective ways to detect disease early, often before symptoms appear.  If you’re due for a mammogram, feel unsure about your options, or want help finding affordable breast cancer screening resources, we’re here to help. Our women’s health team at Raleigh Gynecology & Wellness can guide you to national programs, financial assistance, and the right imaging services with compassion and clarity. Don’t wait to take care of yourself.
If you’re due for a mammogram, feel unsure about your options, or want help finding affordable breast cancer screening resources, we’re here to help. Our women’s health team at Raleigh Gynecology & Wellness can guide you to national programs, financial assistance, and the right imaging services with compassion and clarity. Don’t wait to take care of yourself. Perimenopause often arrives quietly, then all at once. You may notice irregular periods, mood shifts, fatigue, sleep problems, or weight changes that don’t respond the way they used to. This transition lasts an average of
Perimenopause often arrives quietly, then all at once. You may notice irregular periods, mood shifts, fatigue, sleep problems, or weight changes that don’t respond the way they used to. This transition lasts an average of 
 Perimenopause can feel unpredictable, but your daily routines provide grounding and stability. When you support your body consistently through nutrition, sleep, exercise, and stress management, you can gain greater confidence and energy.
Perimenopause can feel unpredictable, but your daily routines provide grounding and stability. When you support your body consistently through nutrition, sleep, exercise, and stress management, you can gain greater confidence and energy. Irregular periods are one of the most common signs of
Irregular periods are one of the most common signs of  One of the most effective ways to stabilize
One of the most effective ways to stabilize 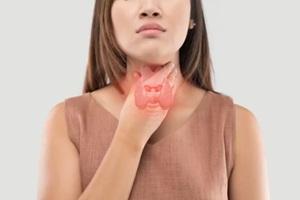 Thyroid disorders
Thyroid disorders