Essential Takeaways:
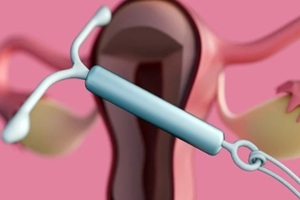 Mild cramping, spotting, and period changes are common in the first few months after IUD placement.
Mild cramping, spotting, and period changes are common in the first few months after IUD placement.- Hormonal and copper IUDs can cause different side effects, especially when it comes to bleeding patterns.
- Most IUD-related symptoms improve as your body adjusts over time.
- Severe pain, heavy bleeding, fever, or unusual discharge should be evaluated promptly.
- Open communication with your women’s health provider can help you feel informed and confident in your birth control choice.
What You Might Experience After IUD Placement
You chose an IUD because you wanted reliable, low-maintenance birth control. It is one of the most effective options available, and for many women it offers years of protection without daily effort. However, after placement, you may notice changes in your body that leave you wondering, “Is this normal?”
It’s common to feel uncertain about what changes to expect after IUD placement. Friends may share stories that do not match your experience, and online forums can increase anxiety instead of offering reassurance. The truth is that most IUD side effects are temporary and manageable. Let’s review some common side effects that often catch women off guard.
1. Cramping That Lasts Longer Than You Expected
Many women expect cramping on the day of insertion, but you might be surprised if it continues for several days or even a few weeks. Mild to moderate cramping is common as your uterus gradually adjusts to the IUD.
Your uterus is a muscle, and it may contract as it adapts to the IUD. For most women, this improves within three to six months. Using over‑the‑counter pain relievers, applying heat, and resting can help reduce symptoms.
If you have severe pain that doesn’t improve, or pain accompanied by fever, call your provider. While rare, complications such as infection or IUD displacement need prompt evaluation.
2. Spotting Between Periods
Unexpected spotting can be frustrating, especially if you chose an IUD for convenience. Light bleeding between periods is a common early side effect, particularly with hormonal IUDs.
The American College of Obstetricians and Gynecologists (ACOG) notes that irregular bleeding is common in the first few months after hormonal IUD placement, gradually getting better in two to six months.
Copper IUDs, on the other hand, are more likely to cause heavier or longer periods, especially during the first several cycles. Research shows that up to 70% of copper IUD users report increased menstrual bleeding in the early months.
Tracking your cycle and keeping a record of bleeding patterns can help you and your provider determine whether what you are experiencing falls within the expected range.
3. Heavier or Lighter Periods

Your period may feel different than what you are used to. With a copper IUD, you might have heavier bleeding and more severe cramps at first and for some women these effects are more persistent. With a hormonal IUD, periods often become lighter and shorter, and in some cases may stop completely.
Up to approximately 20% of women who use a hormonal IUD will stop having periods after one year of use, depending on the IUD brand. This can feel concerning if you are not expecting it, but it is generally safe and related to the thinning of the uterine lining.
If your bleeding becomes extremely heavy, meaning you are soaking through a pad or tampon every hour for several hours, you should contact your provider.
4. Mood Changes or Breast Tenderness
Hormonal IUDs release a small level of progestin in the uterus. While hormone levels in the bloodstream are much lower than with birth control pills and systemic side effects are uncommon, some women do report mood changes, acne, headaches, or breast tenderness.
Not every woman experiences these symptoms, and many notice improvement after the first few months. If mood changes feel significant or affect daily life, don’t ignore them. Open communication with your provider can help determine whether your symptoms are likely related to your IUD or influenced by other factors such as stress or life changes.
5. Feeling the Strings or Partner Discomfort
After placement, your provider will trim the IUD strings so they sit near the cervix. Occasionally, you may feel the strings when checking them, or your partner may notice them during intercourse.
In most cases, the strings soften over time and become less noticeable. If they feel too long or cause discomfort, your provider can adjust them.
It is also important to check your strings periodically, especially in the first few months. Expulsion means the IUD partially or completely comes out. ACOG reports that expulsion occurs in about 2-10% of users. If you cannot feel the strings or think that the IUD may have shifted, schedule an appointment for evaluation.
When Something Is Not Normal
While most side effects are temporary, certain symptoms should prompt you to call your provider. These include:
- Severe abdominal pain
- Fever or chills
- Foul-smelling discharge
- Very heavy bleeding
- Signs of pregnancy or a positive pregnancy test
Remember, if something feels off, it is always appropriate to seek medical advice.
Trust Raleigh Gynecology With Your Contraceptive Care
Choosing an IUD is a personal decision, and your experience should not leave you feeling confused or dismissed. Many side effects are normal and improve with time, but you do not have to manage them alone.
At Raleigh Gynecology & Wellness, we take your concerns seriously. Whether you are considering an IUD, adjusting to a new one, or wondering if your symptoms are typical, we are here to provide thoughtful, individualized care. If you have questions about your IUD or would like to explore your birth control options, schedule an appointment with our team today.

 You probably wear a bra most days without thinking twice. However, stories in the media that claim that underwires could be “bad for your breasts” may raise concerns. Maybe you’ve heard that they block lymph flow, cause chronic pain, or even increase the risk of breast cancer. It’s understandable to wonder if there’s any truth behind these rumors. When it comes to your
You probably wear a bra most days without thinking twice. However, stories in the media that claim that underwires could be “bad for your breasts” may raise concerns. Maybe you’ve heard that they block lymph flow, cause chronic pain, or even increase the risk of breast cancer. It’s understandable to wonder if there’s any truth behind these rumors. When it comes to your  Get fitted regularly. Your body changes over time due to weight shifts, hormones, and aging, all of which can affect breast size and shape. A professional fitting every year or two helps keep your bras supportive and comfortable.
Get fitted regularly. Your body changes over time due to weight shifts, hormones, and aging, all of which can affect breast size and shape. A professional fitting every year or two helps keep your bras supportive and comfortable.
 Hormonal changes and a slower metabolism can result in weight gain, most commonly in the abdominal area, raising the risk of type 2 diabetes and insulin resistance. Balanced nutrition, portion awareness, and regular movement help reduce that risk.
Hormonal changes and a slower metabolism can result in weight gain, most commonly in the abdominal area, raising the risk of type 2 diabetes and insulin resistance. Balanced nutrition, portion awareness, and regular movement help reduce that risk. Menopause marks a new chapter, not the end of health and vitality. By staying proactive with screenings, lifestyle habits, and supportive care, you can protect your well-being for years.
Menopause marks a new chapter, not the end of health and vitality. By staying proactive with screenings, lifestyle habits, and supportive care, you can protect your well-being for years. For many women, the thought of menopause can bring feelings of uncertainty or even worry. It’s a natural transition that every woman experiences, yet the
For many women, the thought of menopause can bring feelings of uncertainty or even worry. It’s a natural transition that every woman experiences, yet the  During menopause, the ovaries stop releasing eggs and produce less estrogen, which can lead to both emotional and physical changes. Common symptoms include hot flashes, brain fog, changes in hair or skin, weight fluctuations, and a decrease in libido. Some women notice shifts in mood or energy levels, while others may experience few symptoms at all.
During menopause, the ovaries stop releasing eggs and produce less estrogen, which can lead to both emotional and physical changes. Common symptoms include hot flashes, brain fog, changes in hair or skin, weight fluctuations, and a decrease in libido. Some women notice shifts in mood or energy levels, while others may experience few symptoms at all. Menopause is a transitional stage in every woman’s life, and with the proper care, it can be managed confidently and comfortably. Embracing each stage and learning how your body responds can help you maintain balance and overall well-being.
Menopause is a transitional stage in every woman’s life, and with the proper care, it can be managed confidently and comfortably. Embracing each stage and learning how your body responds can help you maintain balance and overall well-being. When you come in for breast cancer screening, your
When you come in for breast cancer screening, your 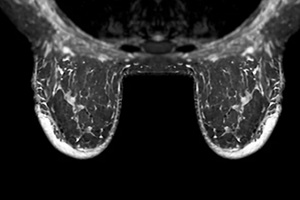 These are reassuring classifications. BI-RADS 1 means no suspicious findings; BI-RADS 2 means there is a benign (noncancerous) feature such as a stable cyst or benign calcification.
These are reassuring classifications. BI-RADS 1 means no suspicious findings; BI-RADS 2 means there is a benign (noncancerous) feature such as a stable cyst or benign calcification. Stay on schedule. If the report calls for follow-up imaging (for BI-RADS 0 or 3), showing up for these
Stay on schedule. If the report calls for follow-up imaging (for BI-RADS 0 or 3), showing up for these